Today we’re talking differences between the Freestyle Libre 3 and Libre 2 (by Abbott), as well as the features, the cost, and which one I prefer after trying both.

So, there are 2 big things happening in the world of metabolic health:
Number one is the rising rates of prediabetes (38% adults) and type 2 diabetes.
Number two is the growing interest in metabolic health even without insulin resistance.
Both require monitoring of blood glucose levels. But only one regularly uses a continuous glucose monitor system.
Can you guess which one? Sadly, it’s not the one with a medical need.
Since TRUEWELL is all about an anti-inflammatory diet and lifestyle, I like to focus on specific conditions that would benefit from this.
And pretty much all insulin resistance conditions fall under that category.
When insulin resistance is present, it’s extremely helpful to know what your blood glucose or blood sugar levels are at all times, and especially after meals. Stress, sleep, and exercise can absolutely affect blood sugar levels as well.
All these factors make wearing a continuous glucose monitor really handy and convenient to keep an eye on how your body responds to these environmental and lifestyle factors, but also to your food.
So, when I got diagnosed with prediabetes I asked my doctor if I could get a prescription for a continuous glucose monitor. For more information on continuous glucose monitors, how they work, how they can benefit you, and how you can get one, catch this post: BENEFITS OF CONTINUOUS GLUCOSE MONITORS AND HOW TO GET ONE.
So starting with the Freestyle Libre 2
I was prescribed the Freestyle Libre 2 continuous glucose monitor, which was the newest available at the time.

So, these things are pretty small, stick to the back of your arm, and track your blood sugar levels in your interstitial fluid.
What I was interested in was that the Libre 3 had been advertised a lot but I had to wait 6 or 8 months for it to actually be released and available at the pharmacy.
So now that I’ve actually used both, I want to share what the main differences are and which I prefer using.
Pros of the Libre 2
So first off, the Libre 2 really is small, it’s about the size of a quarter, maybe, and I believe you can wirelessly attach it to a monitor, but I feel like connecting it to the app you can get on your phone is way more convenient because that’s just one less thing you have to keep up with and most people have their phone on them at all times anyway.

To use the Libre 2, you open the app and tap the Check Glucose or Scan Sensor button and then hold your phone close to the sensor. My phone does a little vibration thing when it’s scanned.
It’s super convenient to be able to see your blood sugar levels at any time, and then keep an eye on them in almost real-time, instead of having to do a finger stick every time.
So this thing makes it really convenient to monitor what food is doing to your body. But if you keep track of even your sleep, stress levels, and exercise as well, you’ll be able to easily start seeing trends in how your blood sugar levels are responding to all those things.

The app allows you to make notes every time you scan for a reading, as well as enter the number of carbs you’re eating or any other notes. I would regularly log exactly what I ate and the order I ate the food so I could see, for example, if eating my protein, fat, and fiber before my carbs mattered.
I have a lot of videos of these types of experiments if you’re interested. Once they’re ready I’ll have them listed in the TRUEWELL channel, so make sure to subscribe to get notifications for these types of videos.
You can also enter a manual blood sugar reading in the log book so you can compare what the sensor is reading and the actual manual readings.
All of this information is available in the portal if you sign up for an account (which is free) on the Freestyle Libre website.
Cons of the Libre 2
What I noticed about the Libre 2 is that there are a LOT of error scans, so sometimes you have to keep doing it until it scans correctly.
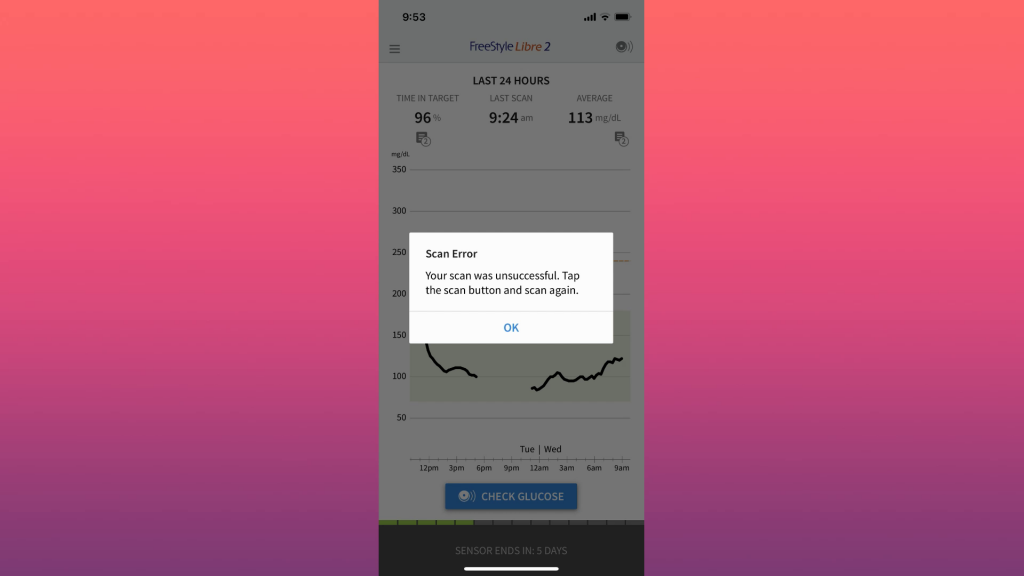
Another thing is that if you put it in a bad place on your arm, it may not even work. I had at least 3 that either were way off in their readings, or wouldn’t scan at all.
This becomes a big inconvenience when you then have to call Abbott and speak to someone for 30 minutes, giving them loads of info on the sensor, just for them to send you a replacement.
I also had a TON of false critical readings with alarms blaring several times during the night. I read up on a few forums and the reviews in the app store and others said the same.

They did an update at one point that I believe allowed you to choose which alarms you wanted, but you can never turn off the most critical alarm. That alarm woke me and my husband up a ton of times before I disabled the app completely every night before bed, so that was super annoying.
Especially when I needed to continue it reading through the night to check on the dawn phenomenon situation.

There were also a LOT of alarms for getting too far away from my phone for it to read. I think there may be a way to disable that as well, I think there were enough complaints about the alarms that they did an update in the app so you have more control over the alarms.

The Libre 2 also comes in the package with 2 separate pieces that you have to line up and put together before you apply the sensor. I’m guessing a lot of people have trouble with this because when I’ve had to call them to have mine replaced, they asked several questions to ensure I didn’t do something other than exactly what the instructions say for putting the applicator together and the actual application process.
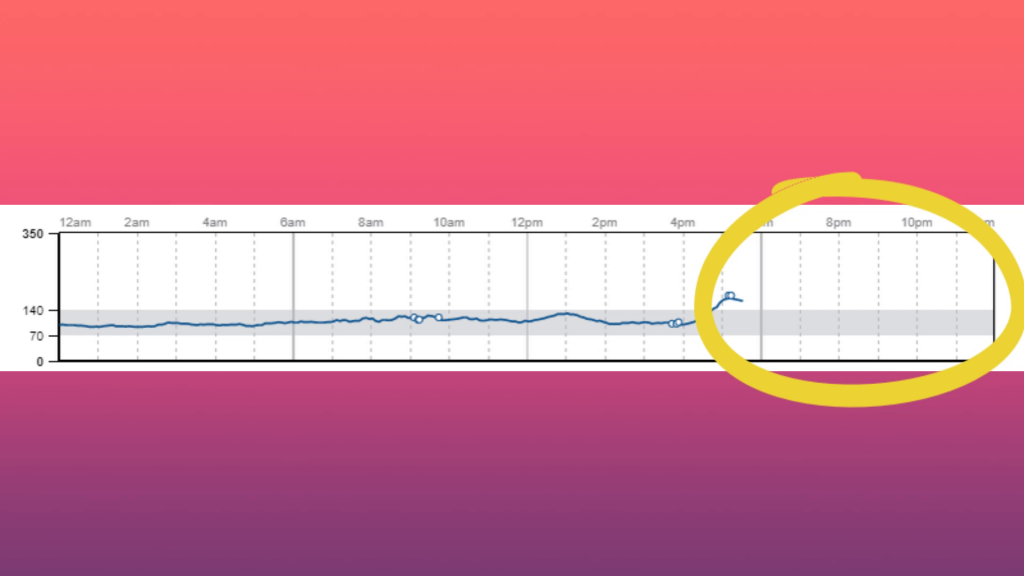
And lastly, if you don’t scan the sensor for 8 hours, there’s a gap in data. That means you MUST scan it immediately before you go to bed, and if you sleep longer than 8 hours there will be a gap.
Same for during the day.
Summary of the Libre 2
All in all, to get started with a continuous glucose monitor, the Libre 2 gave me a ton of information and has made me super aware of how my blood sugar is affected by what I eat.
It’s surprised me many times that things like chips and salsa, or even seed crackers would make my blood sugar spike. And I was eating those things regularly, so it’s no wonder I’ve had a high A1C.
Review of the Freestyle Libre 3
I was super excited for the Libre 3 to come out because it’s got better features than the 2, it’s even smaller, and back last year in 2022 they advertised that it would also monitor ketone levels.
Now that I’ve gotten one and they’ve released it, the part about the ketones is completely missing. The information I read sort of indicated that the next version may have it so my thought is they couldn’t get it accurate or whatever to just get this thing released so they took it out of the description and the app.

The Libre 3 has a totally different app than the Libre 2, but if you have that account online through the Freestyle Libre site, it will connect the two and put all your data in there.

What I love about the Libre 3 is that it’s even smaller than the 2, here you can see the size difference.

This might not seem like a big difference, but I can’t tell you how many times just a millimeter or two of height has caused the Libre 2 to get stuck on bra straps or even the car seat when I’m moving around.
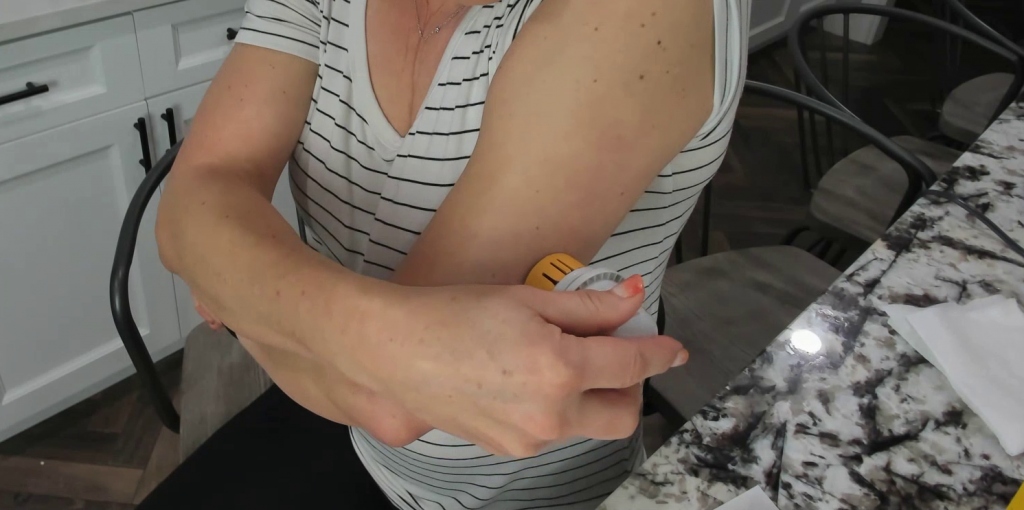
I also love that there’s only one piece in the package. You don’t have to make sure it’s all lined up and then put it together before applying it. They took that component out completely so that applying the sensor is more seamless.
The biggest thing I like about the Libre 3 is the fact that you don’t have to keep scanning it. You do your initial scan when you apply the sensor, then you don’t have to scan it again as long as you stay within about 30 ft of your phone.

This means there are no weird gaps in data like there were with the Libre 2.
This was a big deal for me because I’m constantly trying to figure out what’s affecting my blood sugar at night. I’ve had differences based on types of alcohol and how much I’ve had, plus I had one type of CBD that made it drop really low at night as well.
All of this is important to get to know your body better and be able to make more informed and better choices for your health.
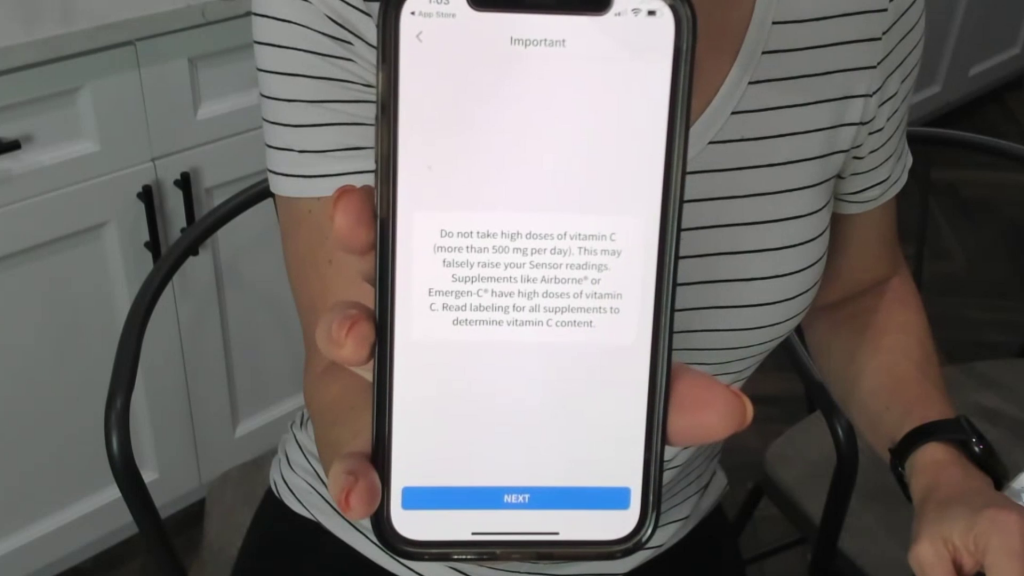
As far as I know, the same disclosures hold true about high doses of Vitamin c and putting a lot of pressure on the sensor.
I also feel like the readings have been more accurate with the Libre 3 than the Libre 2. That’s a big deal because you don’t want to be worried about readings that aren’t really true. Especially when you have to correct with either insulin or glucose.
I don’t really have any cons to list here on the Libre 3.
The one thing that I’ve seen people complain about is they took out the ability to log manual blood sugar checks from the logbook. BUT—I personally don’t really feel like it’s a big deal because at any given time you can add a note like you could in the Libre 2 app and can just enter the manual blood sugar reading there.

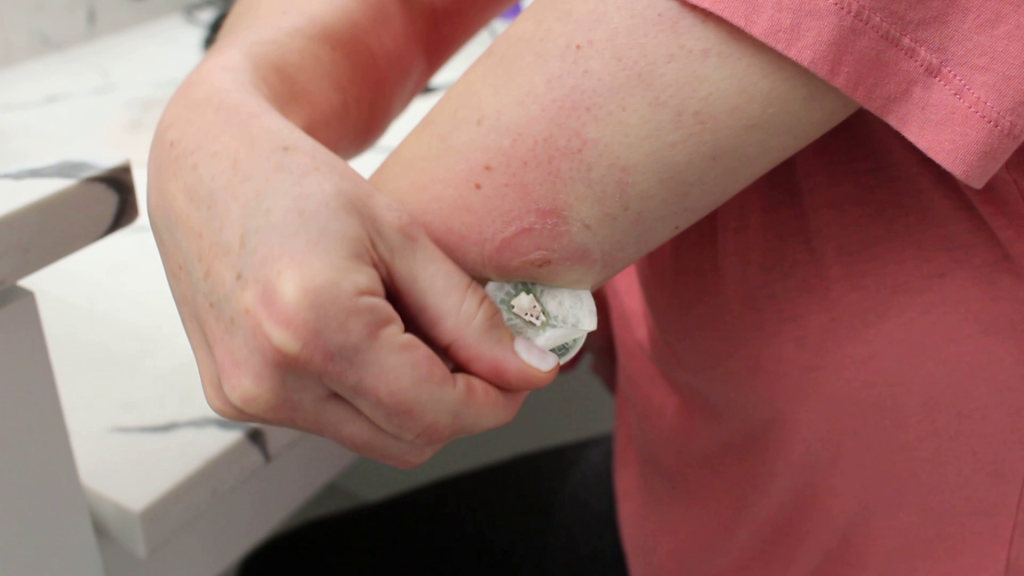
Both have super sticky adhesive, so when you take it off, it feels like peeling a band-aid, so there’s no comparison really on that one.
Price of the Freestyle Libre 3 vs Libre 2
The price is nearly the same for the Libre 3 as it was for the Libre 2.
My insurance doesn’t cover mine because my diagnosis was prediabetes, so I pay out of pocket. For one month it comes out to around $78. If you’d like to know more about how to get one, check out my article that talks all about continuous glucose monitors.
So… all this to say… until a newer better version comes out, I think I’m convinced that the Freestyle Libre 3 is the best option, and that’s absolutely the one I’ll continue to use.
Got more questions? Leave them in the comments below or DM me at: m.me/truewell.co















 QUICK-START GUIDE!
QUICK-START GUIDE!